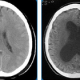
The Subjective Experience of Patients Undergoing Shunt Surgery for Idiopathic NPH
By Jessica Moser
 A recent study out of Yale School of Medicine, led by Dr. Harry Subramanian, looked at the personal experiences of people diagnosed with idiopathic Normal Pressure Hydrocephalus (iNPH). Idiopathic means that there is no known cause of their hydrocephalus. As the symptoms of iNPH are the same as numerous other conditions, it usually takes a lot more testing for doctors to finally reach a diagnosis of iNPH than it does for many other conditions. When a person is diagnosed with iNPH, there is no way to definitely know how their body will react to being shunted or if they will fully return to normal. Therefore, it can be difficult for doctors to appropriately counsel patients.
A recent study out of Yale School of Medicine, led by Dr. Harry Subramanian, looked at the personal experiences of people diagnosed with idiopathic Normal Pressure Hydrocephalus (iNPH). Idiopathic means that there is no known cause of their hydrocephalus. As the symptoms of iNPH are the same as numerous other conditions, it usually takes a lot more testing for doctors to finally reach a diagnosis of iNPH than it does for many other conditions. When a person is diagnosed with iNPH, there is no way to definitely know how their body will react to being shunted or if they will fully return to normal. Therefore, it can be difficult for doctors to appropriately counsel patients.
This study specifically measured patient outcomes and documented each patient’s experience through diagnosis, treatment, and recovery in order to guide clinical counseling. Below are the main outcomes of the study.
The Patient Experience
Education is important. Many of the patients went to several doctors who diagnosed them with everything from dementia to Parkinson’s before being properly diagnosed with iNPH. Those misdiagnosed said that not knowing was the worst part of the whole experience, not the surgery or any of the procedures associated with it. Educating doctors about iNPH as a possible diagnosis that is treatable would potentially help a lot of misdiagnosed people regain functionality and stop their decline.
Most patients wanted the surgery. As soon as it was proposed as an option to treat them, most patients were willing to go ahead with surgery. They didn’t report much difficulty in deciding whether or not to go ahead with it.
People want their lives back. All the patients wanted to be independent again and have improved mobility, and, if shunt surgery would help that, they were willing to have the surgery. Improving their mobility and being able to walk without a fear of falling down was the most important expectation of surgery to all of the patients.
Communication is key. Patients reported significantly less anxiety when there was good communication with the neurosurgeon. Patients also reported less anxiety when they were able to speak to people who had been through the same procedure.
Comorbid conditions can make seeing improvement difficult. Determining whether a patient’s gait has improved if they also have bad knees can be difficult. Any comorbid conditions that have the same symptoms as iNPH can make seeing improvement after shunt placement difficult.
Patients are glad they went through with the surgery. Satisfaction after shunt surgery varied between patients. Some were satisfied with partial recovery or none at all, and some were expecting a full recovery but all were glad they went through with the surgery. Without it, they would never know if it would have helped or not and they would have continued to decline.
Everyone researched the condition and about shunts before the surgery. There was no one source of information that every patient relied on for information. They asked friends and doctors for information and researched online themselves. Having the information helped alleviate some anxiety about the procedure and the condition.
The Clinical Picture
 Symptoms prior to treatment. The surveys found that before treatment, 100% of the people interviewed reported gait changes as a symptom they experienced, followed by urinary incontinence (81%) and cognitive impairments (71%).
Symptoms prior to treatment. The surveys found that before treatment, 100% of the people interviewed reported gait changes as a symptom they experienced, followed by urinary incontinence (81%) and cognitive impairments (71%).
Symptom improvement after treatment. After surgery, 74% of people reported an improvement in gait, 44% in urinary incontinence, and 45% in cognitive functioning.
Complications after surgery. The only complications reported one month after the surgery were headaches, which were reported by 29% of patients, and subdural hygroma (a collection of CSF in between the brain and the protective layer of tissue that surrounds it called the dura) in 10% of the patients.
Why the study is important
It is hard to diagnose iNPH because it can look like many other disorders that come with age such as dementia, and, even after a proper diagnosis, it can be difficult to know which patients will respond positively to shunt insertion. This makes counseling difficult and is exactly why this study is so important. If we know more about what people are thinking and experiencing during treatment, doctors can better accommodate their patients.
The Study Details
Each of the patients had to be over 60 years old, they had to exhibit at least one of the main symptoms of iNPH (gait change, incontinence, or memory problems) and they had to have enlarged ventricles. The researchers in this study interviewed 31 patients over the phone using a semistructured interview format, meaning there was a set list of questions but the interviewer could deviate from the list if they deemed it necessary. They asked questions regarding the patient’s personal experience with iNPH and medical procedures related to the condition such as shunting and lumbar punctures. They collected data such as age and ethnicity from the patient records and specifically asked the patients whether they thought they experienced improvements in characteristics such as their gait or memory.
An abstract of “The Subjective Experience of Patients Undergoing Shunt Surgery for Idiopathic Normal Pressure Hydrocephalus” study is available here.